It's a common question asked after being diagnosed with a lumbar disc herniation or when a patient suspects one.
Can Herniated Discs Heal? from Tom Willemann on Vimeo.
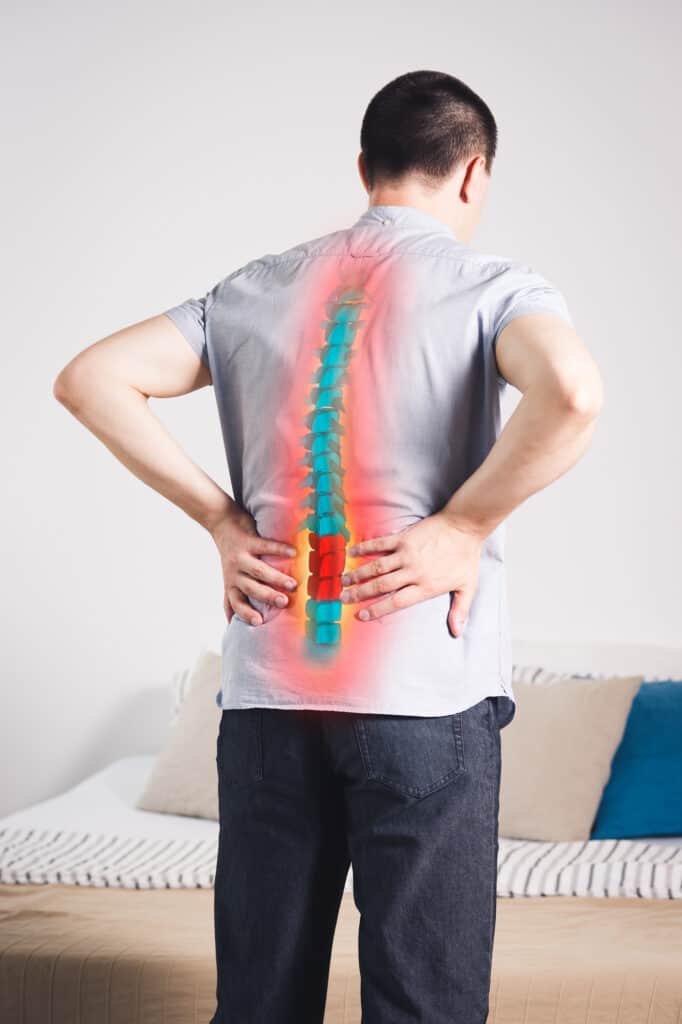
It can be quite upsetting to learn about a disc herniation in your lumbar spine.
Most people who receive this diagnosis have been experiencing lower back pain and many may also report numbness, tingling, achiness, weakness or burning in one or both of the lower extremities.
The good news is that most people will have a complete resolution of symptoms between 6 to 12 weeks which is considered the natural history of this condition.
Simple the passage of time can result in this condition for improving even without receiving care from a physical therapist or other healthcare practitioner.
For those experiencing disc related pain it can persist for an extremely long time so receiving a bit of education from a healthcare provider can alleviate any potential concerns and activities that may delay healing for the individual.
More Articles From Apex
I Have Ongoing Pain In My Leg Muscles; What Can I Do?
Should I Stop Exercising With Knee Pain?
What Is Causing Pain In My Shoulder?
Our Top Tips After Getting A Diagnosis Or Suspecting You Have A Disc Problem:
Avoid bed rest after the first 2-3 days when possible
Excessive bed rest can lead to a longer recovery. The effects of bed rest causing general deconditioning can be huge especially in the older population.
Just moving a little bit more each day or doing simple tasks like making coffee or a short 5 minute walk are essential.
Studies on bed rest have shown in less than 3 days, decreases in cardiovascular function, bone density changes, loss of endurance and muscle atrophy, possible blood clots and depression.
Avoid static postures
Too much sitting, standing, and lying down. We generally recommend changing your position every 10-15 minutes throughout the day as the key to start feeling better.
Maintain a good sleep schedule of 7-8 hours a day
If you aren’t sleeping well taking medications NSAIDs, sleeping pills or pain medications may be necessary but you must consult your doctor first to understand if it is appropriate for you.
Ensure you have proper hydration approximately 8 cups of water a day
Engage in a gentle walking program
Many will not be able to walk any great distance in the early stages of recovery. The goal is 20-30 minutes a day as tolerated.
This is a general rule and listen to your body especially the first few days to gauge your tolerance and reaction after walking.
An alternative strategy is to do the “Meal Plan” walking program by spreading out your walks with short bouts 5-10 minutes for breakfast, lunch and dinner.
Get a physical therapy evaluation
It's important to understand what else you can do so the therapy is personalized for your condition. It is often just as important to know what not to do as what to do.
An individual evaluation of the best exercises of stretching, strengthening or endurance work can make the difference in your overall recovery.
Unless you are experiencing any "red flags" which indicate an immediate MRI.
What Are Red Flags?
Red flags can include progressive weakness, changes in bowel and bladder, and numbness in the region of the perianal region.
If you don't you may try conservative treatment consisting of physical therapy, acupuncture, anti-inflammatories, modification of activities, walking program and ergonomic changes.
Most disc herniations respond to conservative care and don't require more invasive procedures like injections or surgery.
First thing we should discuss is the anatomy of a normal lumbar disc and various types of disc herniations.
The intervertebral discs are complex structures that consist of a thick outer rings of fibrous cartilage called the annulus fibrous, which surrounds the nucleus pulposus that is at the center which is made of water and less dense network of collagen that is commonly to the center of the "jelly donut".
Lastly, the cartilage end-plates of the intervertebral bodies that are above and below the nucleus pulposus and surrounding above annular rings.
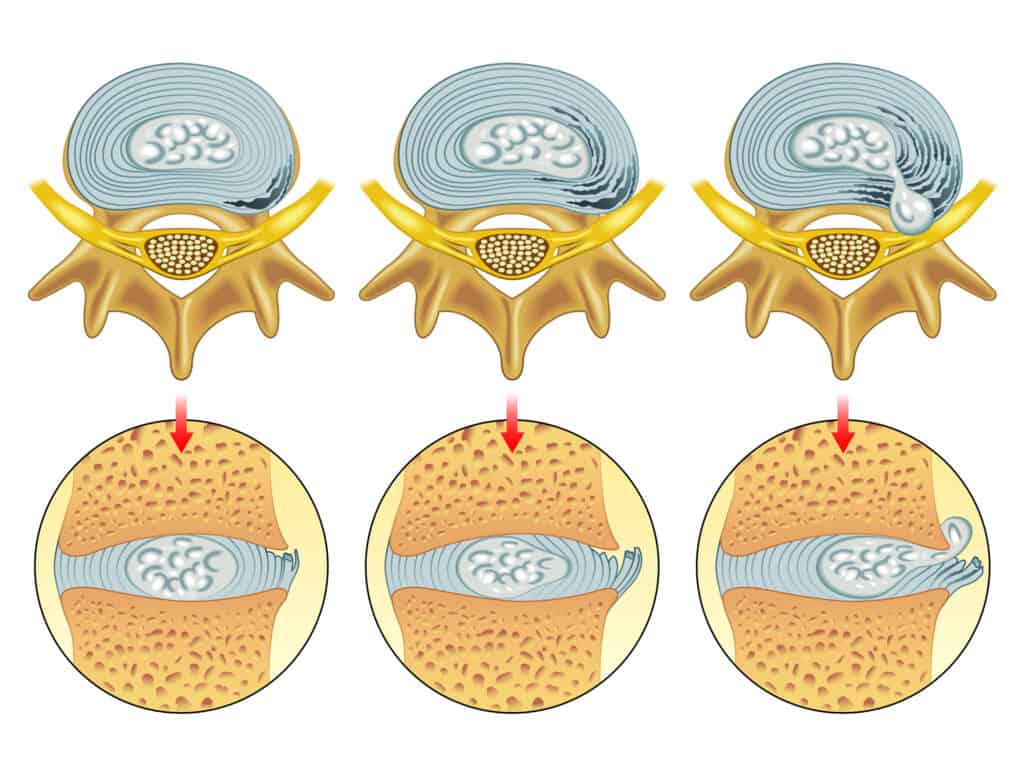
A herniated disc (also called bulged, slipped or ruptured) is a fragment of the disc nucleus that is pushed out of the annulus, into the spinal canal through a tear or rupture in the annulus.
Discs that become herniated usually are in an early stage of degeneration.
What Are The Different Types Of Disc Herniations
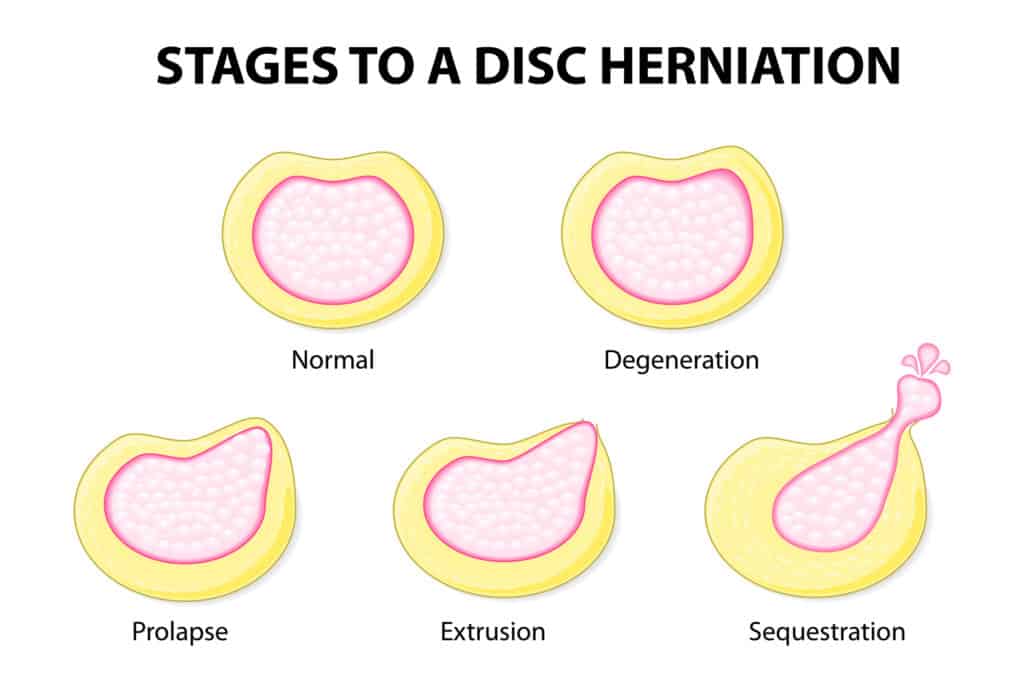
Types of herniations:
If you aren't improving at around 2- 3 months from onset of your condition an x-ray in addition to an Magnetic Resonance Imaging (MRI) may be recommended to visualize the bony and soft tissue structures of the lumbar spine to detect for inflammation, tumor, disc herniations and any soft tissue abnormalities.
The MRI can aid the physician in deciding if a spinal injection is appropriate and what structure may be the "pain generator".
An MRI will rule out more serious pathologies and can be a preparation for surgery when indicated.
Magnetic resonance imaging (MRI) uses a large magnet and radio waves to visualize the soft tissue structures like muscle, ligaments, tendons, nerves, and intervertebral discs.
It is an extremely valuable diagnostic tool in detecting abnormalities in the lumbar spine.
In most cases, an MRI will detect evidence of lumbar disc herniations, but in about 30% of cases there is no evidence of when herniations when followed up during surgery.
This can be related to the gap in time from the MRI until the surgery and reinforces the need conservative care.
In addition, several research studies on MRI of the lumbar spine show patients without a history of back or leg pain or current symptoms show evidence of various types of disc herniations, disc degenerative, spinal stenosis and spondylosis ranging from 50-75%.
With the high number of individuals with abnormal MRIs, a comprehensive physical examination should be used to confirm the diagnosis and possible spinal level in addition to a thorough history from the patient.
What Is The Definition Of A Disc Healing?
Most people believe the absence of pain means the disc has healed.
Once the patient no longer has lower back pain or leg symptoms and has returned to pre-injury activities, these considered indication of a full recovery.
In these cases, the lumbar disc may no longer be a source of pain, but in theory
But may still have evidenced of abnormalities in the disc. It is of considerable debate on what is the current state of a disc when the signs and symptoms are no longer present.
I feel it is safe to say the lumbar disc especially after the more severe herniations like the extrusions and sequestrations it doesn't have the same ability to tolerate certain forces around the spine as compared to a lumbar disc that has no evidence of previous herniations.
Even though in cases of the larger herniations, like sequestrations and extrusions, that are not contained within the annular rings disappear when an MRI is done one year after being.
This spontaneous resolution is thought to be a related to a retraction of the disc material back into the disc annular walls, inflammation that causes the body to attack the disc material as a foreign object causing it be broken down or dehydration of the disc material loses water content.
Since the likelihood of a reoccurrence if high if you have had an episode of low back pain and sciatica, we recommend patients be aware of high risk activities that may predispose them to a second episode.
Each person is unique, so the potential triggers can range from a sedentary job, being a smoker, poor lifting techniques, and obesity.
What Exercises Are Helpful For Those With Disc Herniations And Disc Bulges?

This is a common question for all those recovering from a disc injury.
For patients recovering after a disc herniation from prone press ups and lumbar extensions in standing are the most common corrective exercises, especially if a patient has lost of lumbar extension. Check out these two exercises below for increasing range of motion and hopefully decreasing the time period for disc healing.
In may experience if you are under 50 years of age the prone press-up is typically more effective and the lumbar extension in standing is more effective for those over 50 years of age.
These exercises should be performed 5 times a day for 10-20 repetitions. It is important to spread these exercises throughout the day to maintain your range of motion.
These exercises should never make your condition worse. It is not uncommon to have mild pain while performing them especially at the very end of the range of motion.
As long as your pain levels return to neutral or you actually feel better at the after completion continue to perform for upwards of one week.
If you feel worse your may be doing the exercises incorrectly or it is not the correct exercise for your lumbar disc problem.
There are alternative exercises and modifications of these two exercises that may be necessary.
Only after performing a McKenzie evaluation can by a certified or diploma trained Mckenzie therapist can you truly identify the most beneficial movement or position for your disc related condition.
If you're in pain and want effective treatment today, call us and see how we can help you.


