
More Articles From Apex
What Is Frozen Shoulder?
Take A Walk In A Walking Shoe
Getting To The Route Of The Problem Of Tennis Elbow
After years of running for various sports – from a brief stint with the cross country team at River Dell High School, to my later years participating in triathlons – this question has come up from both patients and fellow athletes often.
People want to know: does running cause arthritis, or make arthritis progress faster than normal wear and tear? In addition to being a runner, I also happen to be a research geek. So let’s get investigating.
Recently, I have been scouring the internet to get an answer to this enduring question. The answer for years (from me) has routinely been that running does NOT cause arthritis, but if you have arthritis, you can progress the arthritis in the knee and hip more rapidly by continuing to run or, in my case, jog slowly.
What Is Arthritis?
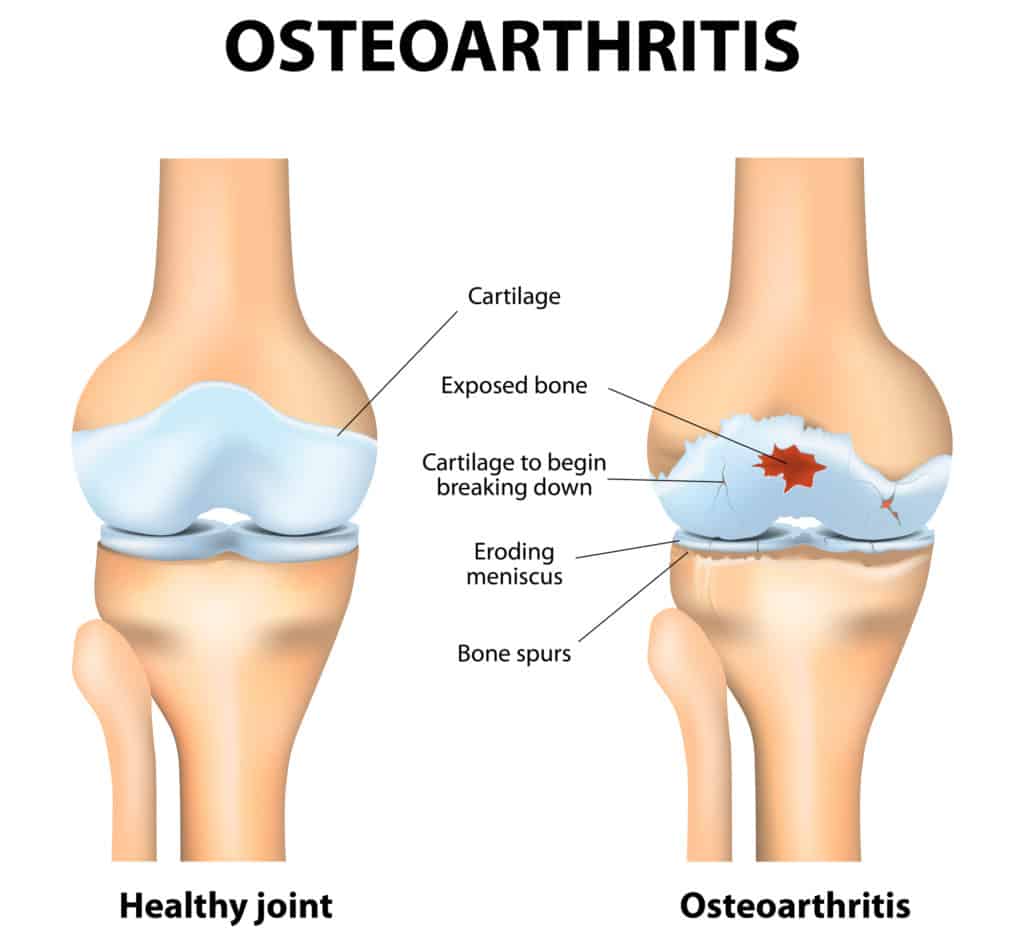
Arthritis is characterized by a deterioration of the joint’s surfaces and rubbing of the normally smooth cartilage causing pain, swelling, stiffness and loss of range of motion and strength of the joint.
When we are born, this joint surface- composed of hyaline cartilage – is smoother than the surface of ice (pretty cool, right?).
Over time, this surface gets rougher and rougher, and eventually breaks down to the underlying bone in severe cases. Over 100 types of arthritis exist, but the most common type is osteoarthritis.
What Are The Risk Factors?
The risk factors that can lead to arthritis include:
History of a previous injury (i.e. joint dislocation, fracture across the joint, meniscal tear, labral tear)
Family history of arthritis
Being overweight > 30 BMI
Age
Occupation or activities that require extensive weight-bearing (i.e. construction, athletes)
Smoking
Does Running Cause Arthritis?

The common view is that the pounding (and repetitive loading) that runners place on joints will eventually wear down the joint surfaces over time, like the front tires of a car.
Apparently, there is no increased risk of developing arthritis between runners and non-runners. However, there are exceptions when looking at elite runners that average greater than 50 miles a week, elite soccer players, and competitive weightlifters and wrestlers.
There is evidence that exercise in general, including running, has a protective effect on the joint by clearing certain chemicals that contribute to joint inflammation and weakening of the cartilage.
The risk-benefit of choosing to exercise versus not exercising is outweighed by the benefits of improving cardiovascular fitness, mitigating stress, maintaining lower body weight, and limiting fall risks.
When comparing individuals with a more sedentary lifestyle, runners overall have other healthy habits that contribute to a lower BMI/make healthier lifestyle decisions, i.e. not smoking, not drinking alcoholic beverages, and overall better nutritional awareness.
That being said, I once had a carpenter as a patient who was an avid runner (5-8 miles a day) that talked about having a small list of friends he would run with. The reason? He routinely grabbed a smoke in the middle of a run!
Obviously being a runner does not guarantee all aspects of your lifestyle are necessarily healthy!
If I Have Arthritis, Will Running Make It Worse?
In the past, I would immediately say “yes” to this question without any hesitation.
Recent evidence by Lo et al 2014 indicates that running may not lead to progressing or accelerating the joint surfaces any more than individuals who are overweight. A study done by Lane in 1993 demonstrated no difference in arthritic changes in runners compared to sedentary individuals.
This is a source of great debate among physical therapists and physicians. My recommendation is to discuss this with your physical therapist for more individualized guidance on starting or returning to a running program.
Ultimately, if you really desire to run as part of a healthy lifestyle, I would recommend gradually progressing your running while monitoring signs of overdoing, since you have the knowledge that the joint is not as resilient as a joint that lacks arthritis changes.
We have experience with athletes that can run with certain restrictions. Once they run too long or don’t allow the knee to recover, it can lead to setbacks.
We see this problem with athletes doing their first marathon, who have been provided with a training schedule with certain goals for each day with progressively increasing mileage.
Once an athlete has a setback during the preparation for the race, they attempt to jump into the same point on the schedule which can lead to overuse injuries or spike swelling in an arthritic joint.
Many of these athletes unknowingly have arthritic changes in their knees or hips even though they don’t have a history of pain, swelling or a history of injury.
If a person is unable to maintain a certain training schedule for a race, or a desire to maintain cardiovascular health, we advocate using a hybrid approach.
A hybrid approach is probably the best strategy that limits excessive joint loading through alternative activities like biking, elliptical, and swimming.
An example of this type of training is: Monday and Thursday are your running days, Tuesday and Friday are your biking days, and Wednesday and Saturdays are your rest days.
Often, we may include light weight lifting for upper and lower body depending on the individual. We may also have to limit certain exercises that load the joint – like squats and lunges from the amount of weight or number of sets.
To really understand your tolerance, a training log is essential to see trends.
For example, every time I squat over 50lbs, I delay my recovery indicated by more pain or joint swelling.
A Few Tips In Order To Run With Knee Or Hip Arthritis
Start a running log. The first thing to start with is logging your runs or jogs via Strava or other software to track your mileage, pace and terrain. Included in this log should be an area to describe how you felt (i.e. knee pain with a rating, swelling or stiffness, took anti-inflammatories).
Most times, especially after an injury, I recommend walk-jog progression.
A simple formula is going to your local high school, which is typically ¼ mile. Start by jogging the straights and walking the parts where the track curves.
Another way is to start with a 5-10 minute run for your first run, followed by two days of rest to gauge a person’s tolerance and the reaction of your joints and your whole body.
Lose a few pounds. The most effective way to lose weight is proper nutrition based on an individualized plan. Start with small changes to your meals and talk to a nutritionist for sustainable and scientifically sound approaches to weight loss.
Losing a pound of body weight can lead to 3-5 times less torque on your knee.
Listen to your body. Everyone has a “sweet spot” where they can run a certain number of days a week, certain mileage, terrain (hills vs. flats), and asphalt compared to cement or a track. If pain, swelling and stiffness follow every run, we need to adjust these parameters and find the right dose of exercise.
Find the correct footwear. Look for a professional who understands runners and types of running shoes. In certain cases, you may benefit from over the counter or custom made orthotics.
Get a physical therapy evaluation. You may need to address the range of motion, strength deficits, weak core or changes to your running form.
Everyone has different ways of moving, but slight tweaks in your form can make a difference in how you tolerate running, especially as you increase your mileage or gear up for a race.
Understand Xray And MRI Imaging With Osteoarthritis
If you have been given a diagnosis of knee osteoarthritis, it doesn’t always mean you have to stop running or jogging.
We have seen recent studies in all areas of the body, from the spine to the knee that indicate arthritis, disc bulges, and tendon tears in individuals who lack pain or impaired mobility.
We have to be careful not to just treat the X-ray or MRI when the pain generator for some may be related to weakness, loss of range of motion, running form or aspects of their training regimen.
The imaging is part of the clinical picture and should not be the only factor when deciding the best course of treatment.
When studies were done using an MRI to check the level of osteoarthritis among people who lacked pain and did not have a history, the rates were 4%-14% in adults aged <40 years to 19%-43% in adults ≥40 years, to quote a study done in the British Journal of Sports Medicine in 2019.
Another conducted by the Arthritis Research & Therapy titled “Aerobic exercise and its impact on musculoskeletal pain in older adults: a 14-year prospective, longitudinal study” looked at pain levels comparing runners who ran 26 miles a week and another group that ran 2 miles a week.
The assumption by many is that they should have more wear and tear. Like wear and tear on an old deck or saw that gets dull, things break down. However, runners that ran 26 miles had 25% less pain than the group that ran 2 miles a week.
Often you will hear me in the clinic saying, “ You can’t treat an MRI!”
If you meet a physician that doesn’t give you time to discuss your history of the condition and check your movements from strength to range of motion, it is time to see another specialist.

A review of the literature has, in some ways, muddied the waters because it is always easier to give a simple answer of “yes” or “no” to this question. Many athletes have visions of their moms, dads or grandparents blaming their current lack of mobility and pain on arthritis.
This further motivates many to ask this question. Arthritis is blamed on multiple joint-related problems way too often. The existence of arthritis on MRI or X-ray imaging can be found in many individuals that have no history of injury, loss of mobility or pain.
The joint changes experienced by many are simply a part of aging and the wrinkles inside your body.
As we have gained more understanding of pain science, we realize the numerous variables that put you at risk for developing joint-related pain.
If you had the time or desire to have multiple healthcare practitioners evaluate your knee or hip, the diagnosis or proposed treatment would vary considerably.
The answers would range from, “You need to work on your range of motion,” to “Your thigh muscles are weak,” to “This is related to poor posture when standing.”
Perhaps it’s an acupuncturist stating, “Your chi is not balanced,” or the nutritionist pointing to a diet too high in simple sugars or, “You need an injection to lubricate the joint or reduce swelling.”
All of these reasons may be true, or a blending of a few…or all of the above.
If you are concerned about running or jogging, check out our free report written by Dr Gil Santos to help you either get started or continue to run pain-free and reach your fitness goals!


